Services

One-on-One & Group Treatments
We’re dedicated to providing our patients with effective one-on-one care in each and every service we provide. Our approach addresses your individual needs and we will have you on the path to rehabilitation and recovery.
At Sports Focus Physiotherapy we have your health and wellbeing top of mind. Take a look at the range of services below.
If you’re unsure of where to start, why not contact us and one of our friendly staff will guide you in the right direction.
Jump straight to a service below
Physiotherapy
At Sports Focus Physiotherapy, we’re dedicated to your well-being through our comprehensive physiotherapy services. Our expert physiotherapists specialise in diagnosing, treating, and providing rehabilitation for musculoskeletal injuries and nerve pain.
Within our Physiotherapy treatments are specific treatments for spinal issues, acute and chronic care, and biomechanical analysis. It’s important to seek help after an injury or if you’re experiencing prolonged pain. Our skilled team of physiotherapists provides expert manual hands-on treatments, tailored to address your specific needs.
We don’t just stop at treatment; we’re here to assist you with work-related activity too. Your recovery is our priority, and we’re committed to helping you regain your optimal physical health and mobility. With a warm and friendly approach, we’ll guide you through your journey to a pain-free and active life.

Sports Physiotherapy
Experience top-tier care with our specialised Sports Physiotherapy services. Sports injuries can occur during any sporting activity or gym session and can be categorised as acute, chronic, or overuse injuries.
Our physiotherapists are skilled in diagnosing and managing all varieties of sports injuries and working with you to help prevent further injury. Whether you’re an athlete seeking tailored injury rehabilitation or an athletic screening, our Sports Physiotherapists can provide you with the attention and care you require.
We also provide more niche services for specific sports. Physiotherapy for Golfers focuses on correct technique, proper equipment, and specific muscle groups. Our Get Fit to Ski program ensures you’re prepared for the slopes by focusing on injury prevention and peak performance.
No matter your sport or level, we understand the unique needs of athletes. Let us help you achieve your athletic ambitions and stay at the top of your game.

Women's Health
Women’s health is of paramount importance at every age, and our Women’s Physiotherapy services are tailored to address the specific needs of women. We offer a wide range of hands-on treatments from our experienced practitioners who have an interest in Women’s Health Physiotherapy, including pre- and post-natal care.
Other key treatment areas include stress urinary incontinence, urgency overactive bladder, pelvic organ prolapse, pelvic pain, and irritable bowel syndrome. With a warm and friendly approach, we provide a safe space for you to discuss your concerns and receive the care you deserve. Your health and comfort are our priorities, and we’re here to assist you every step of the way.
Women’s health physiotherapy is available at Northbridge, Liverpool and Castle Hill.

Exercise Physiology
Exercise Physiologists help manage and prevent chronic diseases and injuries through evidence-based exercise prescription. Alongside exercise, we provide education and support for different populations to promote healthier lifestyle changes. We also provide performance management for athletic populations to enable sports people and athletes of all types to reach their full potential.
Our Exercise Physiologist treats at Sports Focus Physiotherapy Mounties and MacArthur.

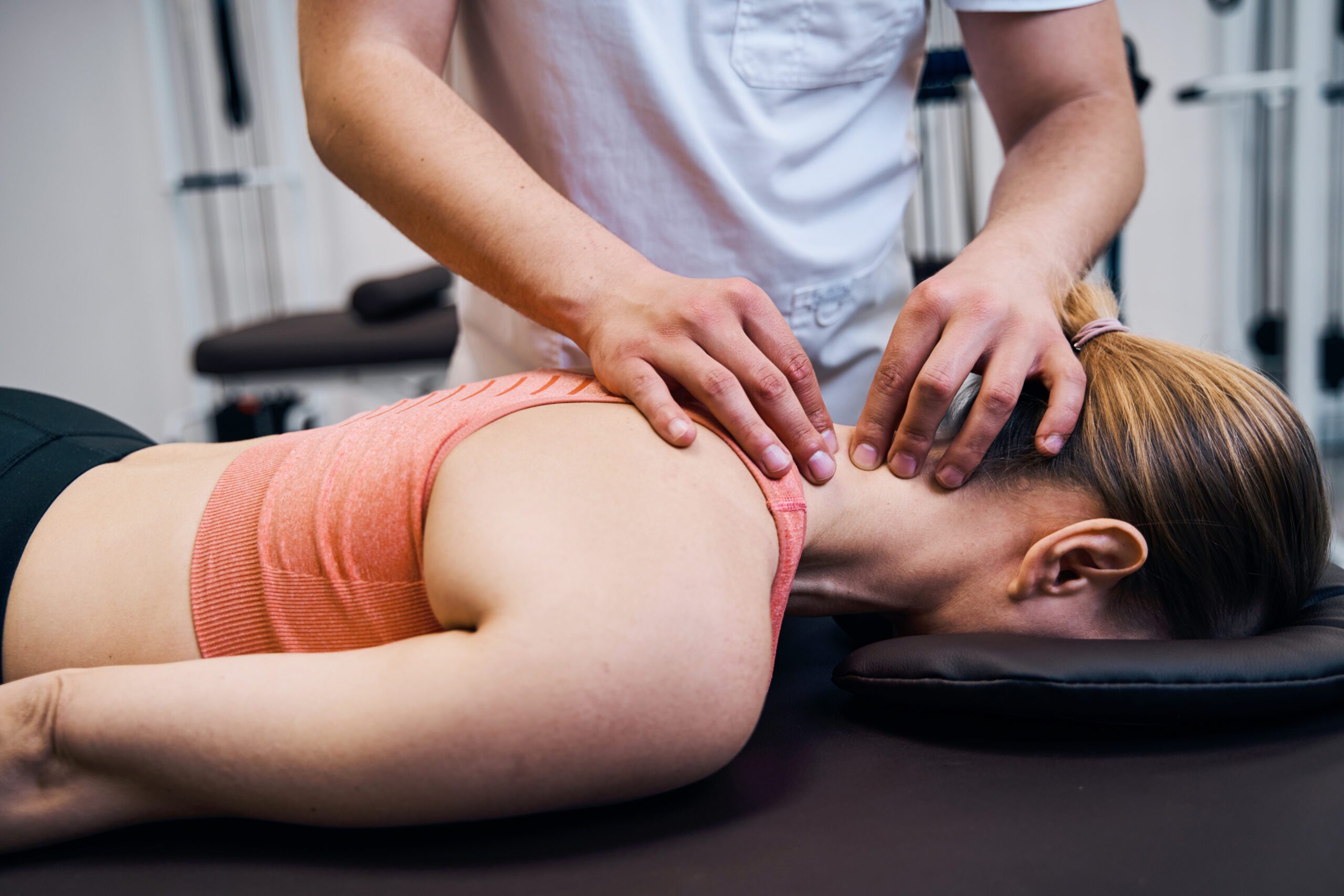
Massage Therapy
At Sports Focus we have experienced Massage Therapists who work to restore optimal function, wellness and health through various types of massage therapies. Relaxing and restorative or remedial and injury specific our therapists can help.
Massage therapy is offered at our Castle Hill, Liverpool, and Northbridge locations.
Active Physio Pilates
Pilates classes tailored by our Sports Focus Physiotherapists. These classes are for all levels – beginner, intermediate or advanced. They are designed by our experienced clinical Pilates Physiotherapists with their background in muscle and joint rehabilitation exercises for all ages. You can find our pilates classes at out Castle Hill and Northbridge clinics.

Aquatic Physio/Hydrotherapy
Aquatic Physiotherapy is a tailored programme of exercises and mobilising techniques prescribed and monitored by an Exercise Physiologist or Physiotherapist. Programmes are conducted on a 1-on-1 basis at our Mount Pritchard clinic.
Aquatic physiotherapy uses the buoyancy and resistance of water to decrease pain and swelling, increase function, strength and range of movement. It is helpful for orthopaedic, spinal and arthritic conditions as well as sports injuries, work related injuries and neurological conditions.

Vestibular Physiotherapy
Vestibular conditions can cause symptoms such as vertigo, dizziness, imbalance, nausea and fatigue. Physiotherapists trained in vestibular rehabilitation will perform a thorough assessment to correctly diagnose the cause of your symptoms which can help determine whether physiotherapy may benefit or referral to a medical practitioner is indicated for further investigation.
Vestibular physiotherapy is offered at our Liverpool and Macarthur locations.

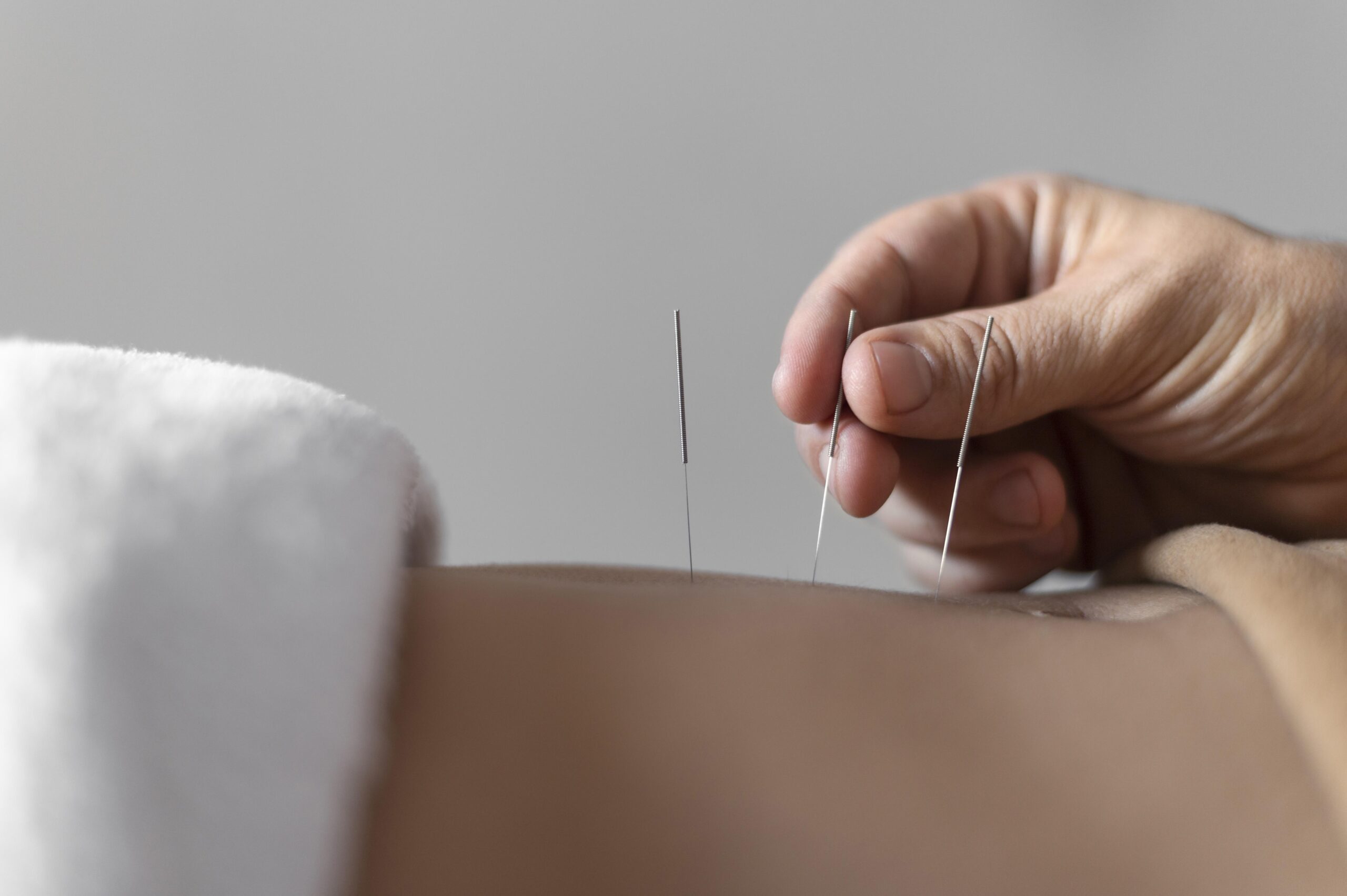
Dry Needling
Dry needling is a useful and effective technique using fine filament needles which are inserted into the fascia or muscle to correct imbalances within the tissue. Often, we target the active trigger points which elicit a twitch response and allow the muscle to release and relax. It can also be used to stimulate a weak or inactive muscle.
It can be used in the treatment of muscular pain, myofascial dysfunction, tendonitis, tension headaches and back pain.
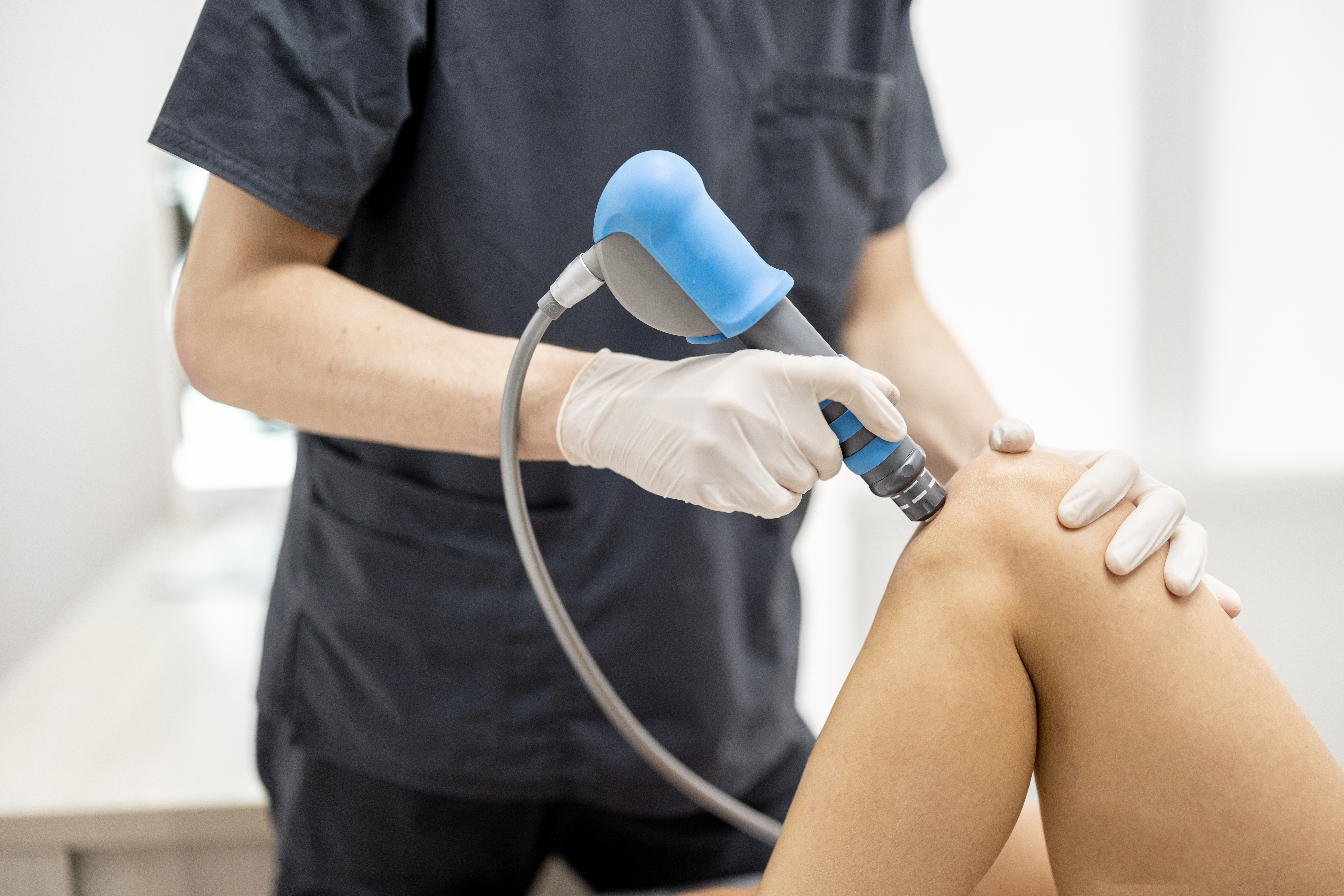
Shockwave Therapy
Shockwave is a safe, non-invasive physiotherapy modality that effectively treats a variety of musculoskeletal conditions. It can be a great alternative to surgical intervention, and can often treat stubborn, recalcitrant conditions.
Shockwave Therapy is done in conjunction with a suitable physiotherapy program, such as an exercise or loading program, and any manual therapy.
Shockwave therapy is offered at our Northbridge, Liverpool, Castle Hill and CBD Wynyard locations.
Adjunct Therapies
At Sports Focus Physiotherapy, we offer a range of adjunct therapies to complement your treatment. From kinesio taping and sports taping to orthotic prescriptions, casting, and splinting, our services are designed to provide comprehensive care for your needs. Our professional team ensures that you receive the best possible care to aid your recovery and improve your quality of life.
We approach every patient with a friendly and caring attitude, ensuring that your journey to wellness is as comfortable and effective as possible. Trust us to provide you with the adjunct therapies you need to support your recovery and enhance your overall well-being.

Naturopathy
At Sports Focus Physiotherapy, our naturopathy services aim to treat the underlying causes of disease and promote overall wellness. Our naturopathic practitioner prescribes complementary therapies tailored to each patient’s needs, including nutritional supplements and herbal medicine. With a focus on digestive disorders, stress, allergies, fatigue, and weight loss, our naturopathic treatments can help you achieve optimal health and well-being. Take the first step towards a pain-free and active life by booking a consultation with our dedicated team today.

Spinal Physiotherapy
Spine-related pain is incredibly common, affecting most of us at some point in life. It can strike various areas like the neck, upper back, lower back, or pelvis. Fortunately, physiotherapy offers effective solutions for managing and alleviating back pain.
Whether you’re dealing with office-related neck discomfort or sudden pain from bending or lifting, our skilled physios at Sports Focus are here to assist. We specialise in biomechanical assessments and tailored treatments to restore your spine’s natural function. Say goodbye to pain and hello to a healthier you!

Pre-Post Natal Physio
Make an appointment for 2 weeks after delivery with our experienced Women’s Health Physiotherapists.
At Sports Focus Physio, we can examine and assess: Breast problems from feeding – Mastitis; Abdominal /scar examination – Diastasis Rectus Abdominis (DRA) assessment; Pelvic Floor Muscle (PFM) assessment; Prolapse assessment; and Postural and Pelvic / lumbar spine assessment
Early assessment and advice are really valuable for a good safe recovery and return to exercise.

Casting and Splinting
Sports Focus physiotherapy can help you manage fractures and injuries that require casting, bracing or splinting.
This service is available for people of all ages and includes the application and removal of casts, moulding thermoplastic splints and fitting braces across a wide range of joints in the body.
We use a fiberglass casting material with the option for a waterproof Delta-Dry liner, which allows the water to pass through the cast, has great ventilation properties and dries very quickly.

Biomechanical Analysis
The human body is complex and has many moving parts. At Sports Focus, our physiotherapists have a great understanding of the body’s anatomy and can identify biomechanical patterns or faults within the system.
Whether you’re recovering from an injury or aiming to reduce your risk, a biomechanical assessment can determine areas of weakness or tightness so that a tailor-made exercise program can be created to your specific requirements.
The biomechanics of the human body can be viewed in many different functional tasks such as walking, running, squat and overhead lifting. Whether you are struggling with repetitive injuries, poor posture or trying to ensure your body is working optimally for your sport; a biomechanical assessment can help you to achieve your goals safely.

Acute And Chronic Care Physiotherapy Rehabilitation
It is never too early or too late to visit a physiotherapist!
Acute care
It’s important to seek help after any injury. Here at Sports Focus Physio, our Physio’s can assess your problem and decide on suitable immediate treatment or referral on for further investigations.
We can provide you with early support for soft tissue injury or mobilisation for stiff and painful joints. An exercise program tailored specifically to your injury will assist with quick recovery.
Chronic Injury/problems
Physiotherapy treatment is very effective in the later stages of a soft tissue injury or chronic joint problem.
At Sports Focus Physio we are experienced in rehabilitation of long-term sporting injuries (such as ACL reconstructions), post-operative joint replacements, as well as ongoing management of degenerative injuries such as osteoarthritis.
A mix of hands-on treatment as well as an independent exercise program will be tailored to meet your needs until you have returned to your pre-injury ability and promote ongoing self-management.
Acute care and chronic physiotherapy and rehabilitation is offered at all our Sydney physiotherapy locations.

NordBord Rehabilitation
Our NordBord is a special piece of equipment that focuses on strengthening athletes’ hamstring muscles through different exercise techniques.
At Sports Focus Physiotherapy we specialise in providing programs that focus on strengthening muscles for athletes in premium teams, to help prevent injuries before they occur.

Telehealth
For those of you who are ‘physically isolating’ at the moment we can still help, even if you can’t come into see your Physio.
TeleHealth allows you to gain remote access to our experienced practitioners from your phone or device.
Get the physiotherapy treatment you need from the safety of your own home.

Kinesio-Taping
Kinesiology tape (K-tape, kinesio tape, rocktape, dynamic tape) is a form of stretchy sports tape that’s used to dynamically assist muscle function without restricting any range of movement. Our physio’s can use kinesio tape with most athletic injuries and a variety of physical disorders in all phases of rehab.
For example, K tape can be used in early post-operative rehab, muscle injuries or in late-stage rehab assisting return to sport exercises.

Manual (Hands-On) Physiotherapy
Manual therapy is a “hands on” approach to the body’s joints and soft tissue structures in order to restore normal function.
Our highly qualified clinicians are experienced in delivering various methods of manual therapy tailored to everyone, including shoulder physiotherapy, neck physiotherapy and women’s health physiotherapy.
With the use of palpation, our therapists are skilled in identifying whether these structures are abnormally tight, in spasm or in some cases hypermobile (too much movement).
Manual therapy can be practiced on all regions of the body.

Athletic Screening Pre-Season
The purpose of a musculoskeletal athlete screen is to develop a clinical picture of an athlete’s capability regarding their sport.
Athletes require strength, range of motion and co-ordination, not only to maximise their performance, but reduce the risk of injury.
During the screening process the athlete is asked to perform a battery of tests and the results of these tests are compared to normative values to identify areas which may place the athlete at risk of injury.
Injury prevention should be the top priority for all athletes to maximise their performance, and longevity of their sporting careers.

Work Related Activity Programs
Work related activity programs are designed specifically for the injured worker depending on their injury and the duties needed to be performed at work.
Our therapists provide education on injury management and prevention and provide the foundations to return to work through a range of exercise techniques.
Hydrotherapy, home exercise programs and gym programs are used to promote self-management and adherence for the injured worker.
Senior Physiotherapy Services
Our Senior services are one-on- one programs designed to improve senior wellbeing and independence.
After an assessment, our Physios can recommend either an individual treatment program or one of our ‘classes’ that specialise in Senior’s health. These include:
- Falls prevention
- Strength and Mobility – cardiac & respiratory
- Balance and Bones

Real Time Ultrasound
Real time Ultrasound uses a diagnostic ultrasound machine to build an image on the screen.
Different layers of muscles can be viewed to see how they contract, relax and work together.
This is very relevant for your “deep abdominal muscles “core” Transverse Abdominus.
It is common for these deeper muscles to not work correctly after any episode of Back or Pelvic pain.
Balance And Bones
Research has shown that elderly people who participate in a safe exercise program that combines both strength training and balance are less likely to have fall related injuries and will improve overall strength.
At Sports Focus Physiotherapy, our Balance and Bones exercise class is conducted by experienced physiotherapists who will take you through a range of safe exercises each session.

Golf Performance
Sports Focus Physiotherapy at Castle Hill offers specialised services for golfers, including rehab and advice for golfing injuries and a golf performance program.
Whether you are playing at professional or amateur, senior or junior levels, our expert Sports Focus physiotherapists can help you get the most out of your game.

Sports Taping
Do you work in the fitness industry? Interested in learning kinesiology taping techniques to help prevent client injury?
Andrew Hughes, senior partner at Sport Focus Physiotherapy and Sports & Olympic Physiotherapist regularly conducts certified taping courses for the sporting community including coaches, athletes and parents at our practices across Sydney.

Orthotic Prescriptions
Orthotics are shoe inserts that support the foot. They are designed to assist in changing gait abnormalities that are causing pain or discomfort.
Orthotic prescription can be done after a biomechanical assessment by your Physiotherapist to determine your individual needs. First steps will often involve taping and sometimes shoe prescription to help change problematic movement issues.
Orthotic prescriptions are offered at all our Sydney physiotherapy locations.

General Physiotherapy For All Client Types
We provide general physiotherapy treatments to patients of all ages. Doctor referral is generally not necessary for private self-pay clients and our HICAPs system can provide you on-the-spot private health fund claiming.
Our physiotherapists also collaborate with your GP, other allied health professionals or insurance company when providing physiotherapy services via Department of Veterans’ Affairs (DVA), Medicare Chronic Disease Management (CDM) program, workers compensation or third-party insurance claims.

Get Fit To Ski
Skiing and snowboarding both demand a lot from the muscles in the quads and lower back, and from the knees. A good conditioning program should start long before the snow season starts, and involve strength, power, flexibility, endurance and agility drills.
Evening classes run in two seasons – pre-Australian season and pre-Northern hemisphere season, 8-10 weeks, one hour.

Move Better Today
Trust our dedicated team to provide valuable support in enhancing mobility, reducing discomfort and get you back to your best.

PHYSIOTHERAPY
Hydro/Aquatic Physiotherapy
Sink into the healing benefits of Aquatic Physiotherapy, also known as Hydrotherapy, in our specialised group or individual classes. Held in the Bundaberg Swim Academy heated pool, these sessions offer a unique approach to rehabilitation and exercise.
The water’s buoyancy supports your body, reducing strain on joints and allowing for gentle yet effective movement. Our experienced physiotherapists guide you through a range of exercises tailored to your needs, targeting strength, flexibility, and balance.
Whether recovering from an injury or seeking low-impact workouts, our Aquatic Physiotherapy classes provide a refreshing and effective way to improve your overall well-being. Join us and experience the therapeutic power of water.
Please note that an in-rooms consultation is required before joining a group session. This allows assessment of injuries and health issues, enabling our Physiotherapist to create personalised exercise programs for each participant.
Time:
Friday 8:00am-9:00am
$95 for initial consultation
$105 for one on one sessions
$20 for group pool classes (pool entry not included)
Frequently Asked Questions
Physiotherapy can treat a wide range of conditions and injuries, including:
Musculoskeletal conditions: Back pain, neck pain, joint pain, arthritis, tendonitis, sprains, strains, and fractures.
Sports injuries: Ligament tears, muscle strains, overuse injuries, and post-surgical rehabilitation.
Postural and ergonomic issues: Poor posture, workplace injuries, and repetitive strain injuries.
Women’s health issues: Pelvic floor dysfunction, pregnancy-related pain, and incontinence.
Geriatric conditions: Age-related mobility issues, balance problems, and falls prevention.
Post-operative rehabilitation: Facilitating recovery after surgery or as an outpatient.
Chronic pain management: Fibromyalgia, complex regional pain syndrome (CRPS), and chronic headaches.
It’s important to note that this is not an exhaustive list, and physiotherapy can be beneficial for various other conditions and injuries. Consulting with one of our physiotherapists is the best way to determine the suitability of treatment for needs.
During your first physiotherapy appointment at Quay Street, you can expect nothing but friendly, dedicated and respectful staff with expert treatment. A typical consult may look like the following:
Initial Assessment: The physiotherapist will conduct a thorough assessment of your condition, including asking questions about your medical history, symptoms, and any previous treatments.
Physical Examination: The physiotherapist will perform a physical examination to evaluate your range of motion, strength, flexibility, posture, and any specific tests related to your condition.
Diagnosis and Treatment Plan: Based on the assessment findings, the physiotherapist will provide a diagnosis and discuss a customized treatment plan tailored to your needs and goals.
Treatment Techniques: The physiotherapist may utilize a variety of treatment techniques such as manual therapy, exercise prescription, electrotherapy, heat or cold therapy, and other modalities specific to your condition.
Education and Advice: The physiotherapist will educate you about your condition, provide advice on self-management strategies, and offer guidance on exercises and lifestyle modifications to support your recovery.
Goal Setting: Together with the physiotherapist, you will establish realistic goals for your rehabilitation journey, focusing on restoring function, reducing pain, and improving overall well-being.
Follow-up Appointments: The physiotherapist may recommend a series of follow-up appointments to monitor your progress, modify the treatment plan if needed, and provide ongoing support.













